Pumping Without Losing Your Mind: Flange Size, Schedules, and Output
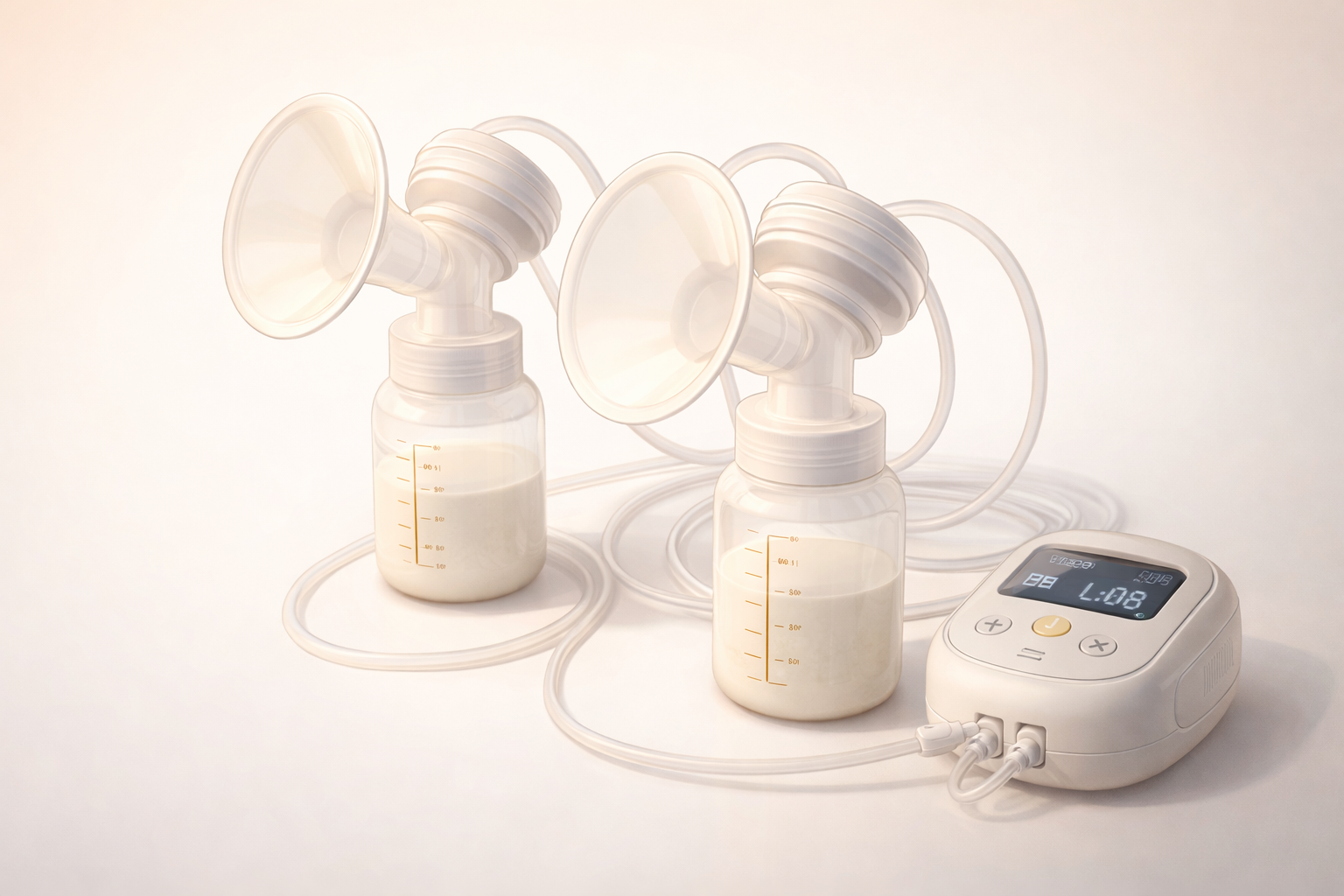
Pumping With a Newborn: The Hobby Nobody Asked For (But Here We Are)
Pumping is one part feeding, one part engineering, and one part “why is the dishwasher full again?”. You finally sit down, assemble the parts, attach yourself to the machine… and your baby chooses that exact moment to request:
- a cuddle
- a diaper change
- a full Broadway performance
- and possibly a small committee meeting
If you’re pumping—whether occasionally, regularly, or exclusive pumping—this post is your friendly, practical guide to:
- building a pumping schedule newborn life can realistically follow
- picking the right flange size (yes, it’s that important)
- troubleshooting low pump output without spiraling
- and (your conversion-friendly piece!) creating a simple pumping station and parts-drying workflow so pumping doesn’t take over your kitchen, soul, and counter space
Start at our feeding hub for the full series: Feeding Hub
Newborn feeding basics: How to Survive Newborn Feeding?
If you’re mixing breastmilk and formula (or breast and bottle), see Newborn Combo Feeding
First, a Reality Check: Pumping Isn’t “Easy Mode”
Some people pump because breastfeeding isn’t possible or isn’t working right now. Some pump because it gives flexibility. Some pump because they want to share feeds. Some pump because their nipples are currently writing a strongly-worded letter. All of those reasons are valid.
And if you’re staring at your bottles thinking, “Is this enough?”—remember:
- pump output is not a moral score
- early weeks are often lower and more variable
- time of day matters
- stress and sleep matter (unfair, but true)
- “enough for your baby” is the goal—not “enough to fill a chest freezer and impress strangers”
The 3 Levers That Make Pumping Easier (and Improve Output)
1) Flange size (comfort and milk removal)
Wrong size can cause pain and reduce output.
2) Frequency (milk removal drives supply)
Especially in the first 6–12 weeks, how often you remove milk matters a lot.
3) Workflow (station and drying system)
This is the “not losing your mind” part. Because pumping is already work—your setup shouldn’t add a scavenger hunt.
Flange Size 101: The Most Underrated Output Fix
Let’s talk flange size—the plastic funnel that can quietly make pumping feel easy… or feel like sandpaper.
What a good flange fit looks like
During pumping:
- nipple moves freely in the tunnel (not rubbing)
- minimal areola is pulled in (some is okay, a lot usually isn’t)
- no pinching, burning, or “shaving sensation”
- nipple looks normal afterward (not flattened or angry)
Signs the flange is too big
- too much areola being pulled into the tunnel
- nipple swelling dramatically
- decreased output
- friction at the base of nipple
Signs the flange is too small
- nipple rubs the tunnel walls
- pinching/burning
- blanching (turning white) after pumping
- poor flow even when you should be letting down
Quick “try this today” tip
If pumping hurts or output is unexpectedly low, flange size is one of the first things to troubleshoot. Many people need smaller flanges than what comes in the box. If you can, use:
- a printable nipple ruler
- a pump brand sizing guide
- or an IBCLC for sizing help
Pump Settings: Stronger Isn’t Always Better
A pump is not a video game. You do not win by leveling up suction until your eyes water. Most pumps have:
- stimulation/letdown mode (fast cycles, lighter suction)
- expression mode (slower cycles, stronger suction)
A simple pumping routine
- Start in stimulation mode until letdown (often 1–3 minutes)
- Switch to expression mode
- Increase suction to “strong but not painful”
- If flow slows, briefly return to stimulation mode to trigger another letdown
If you’re in pain, adjust flange size and suction before changing your schedule.
Pumping Schedule Newborn: The Templates That Work in Real Life
Newborns eat frequently. If pumping is the main milk source, the early schedule can feel intense—but it can be structured in a way that’s survivable.
If you’re exclusively pumping (EP) for a newborn
A common target early on: 8–12 sessions per 24 hours. Yes. That’s a lot. The goal isn’t perfection; it’s consistent milk removal while your supply is establishing.
Sample EP schedule (8 sessions):
6am ➡️ 9am ➡️ 12pm ➡️ 3pm ➡️ 6pm ➡️ 9pm ➡️ 12am ➡️ 3am
Why it works: Steady spacing, protects supply without being “every two hours forever”.
Sample EP schedule (10 sessions):
6am ➡️ 8:30am ➡️ 11am ➡️ 1:30pm ➡️ 4pm ➡️ 6:30pm ➡️ 9pm ➡️ 11:30pm ➡️ 2am ➡️ 4:30am
Why it works: Higher frequency can help if output is low early on.
If you’re pumping in addition to nursing
Your schedule depends on your goal. Common options:
- 1 morning pump (often highest output)
- pump after a feed if baby didn’t nurse long or breast still feels full
- pump during a missed feed if baby takes a bottle instead of nursing
If you’re combo feeding (Breastmilk and Formula)
Combo feeding can reduce pressure, protect sleep, and still give baby breastmilk benefits. It’s a strategy, not a surrender. Read more here Newborn Combo Feeding.
How Long to Pump Each Time?
Most people land somewhere around:
- 15–20 minutes per session early on
- sometimes 20–30 minutes if letdown is slow or supply is still building
A practical approach is pump until milk slows, then continue 2–5 minutes to encourage fuller emptying. If longer pumping makes things worse (pain, swelling, less output), revisit flange size and suction.
Low Pump Output: The Calm Checklist (No Doom-Scrolling Required)
If you’re dealing with low pump output, start here—step by step.
Step 1: Check timing and consistency
- Are you going too long between sessions?
- Is baby sleeping longer and your schedule didn’t adjust?
Step 2: Check flange size and comfort
Pain and swelling often = poor milk removal.
Step 3: Replace pump parts
Worn valves/membranes can quietly tank output.
Step 4: Add hands-on pumping
Massage before and compress during pumping. This can help milk flow and increase output for many people.
Step 5: Improve letdown
Try:
- warmth before pumping
- shoulders down and slow breaths
- looking at baby or a photo/video
- a consistent routine (your brain loves “same steps, same place”)
Step 6: Respect time-of-day biology
Many people pump more in the morning and less in the evening. That’s common and not a sign you’re failing.
Step 7: If needed, adjust frequency (temporarily)
Sometimes the most effective fix is adding a session or doing power pumping for a few days.
Power pumping (short-term tool)
1 time/day for a few days:
- pump for 20 minutes
- rest for 10 minutes
- pump for 10 minutes
- rest for 10 minutes
- pump for 10 minutes
Not mandatory. Not forever. Just a tool.
Exclusive Pumping: How to Make It Sustainable (Not Miserable)
Exclusive pumping is absolutely a valid feeding path. It’s also logistically intense—so your systems matter.
What makes EP easier fast
- a pumping bra that fits
- multiple pump part sets
- a consistent station and drying workflow
- simple storage labels
- an “I am not doing everything today” mentality
Build a Simple Pumping Station and Parts-Drying Workflow
Here’s the thing: pumping gets exponentially easier when you remove friction. If you have to hunt for parts, clean space, find a towel, find a bottle, find a cap… you’ll dread every session.
A pumping station is basically saying: “Future me deserves fewer problems”.
Your Simple Pumping Station (10 items, one spot)
Pick a location you can reliably pump (bedside, couch-side, or kitchen-adjacent). Put everything in one bin/caddy.
Station checklist:
- Pump and power cord/charger
- Extra set of valves/membranes (tiny parts that ruin everything when missing)
- Flanges (your correct sizes)
- Pumping bra
- Burp cloth or small towel (spills happen)
- Water bottle with a straw lid (hydration is not optional)
- Snacks you can eat one-handed
- Phone charger / long cable
- Milk storage bags or bottles and caps
- A Sharpie and labels (or masking tape)
Bonus sanity items:
- hand cream (washing parts will age your hands 12 years)
- a small trash bag (used pads/tissues/wrappers)
- headphones for shows/podcasts (pumping time = entertainment tax refund)
The Parts-Drying Workflow (the “no more wet parts on every surface” system)
Your goal: Wash → Dry → Store without chaos.
Option A: The “Dedicated Drying Rack” System (recommended)
What you need:
- a dedicated bottle/parts drying rack
- a small basin/bin for washing (so parts don’t touch the sink)
- a clean towel or mat under the rack
Workflow:
- After pumping, do a quick rinse (if you can)
- Wash parts in your basin with hot soapy water
- Air-dry on the rack
- Once dry, store parts in a clean bin or drawer right beside the rack
Why it works: Parts always live in one place. Dry parts don’t migrate across your kitchen like tiny plastic tumbleweeds.
Option B: The “Two-Set Rotation” System (best for EP)
What you need:
- 2–3 sets of pump parts
Workflow:
- Set 1 in use
- Set 2 clean/dry and ready
- Set 3 “in wash” (optional)
Why it works: If you can’t wash immediately, you still have parts ready. This prevents the dreaded “I can’t pump because the parts are wet”.
Option C: The “Night Stand Kit” System (for overnight pumping)
What you need:
- small bedside bin with: clean flanges, valves, bottles, caps, wipes/towel
Workflow:
- everything you need at night stays in the bin
- in the morning, carry the entire bin to the wash station
Why it works: Middle-of-the-night pumping should not require a scavenger hunt.
When to Get Help (IBCLC and Beyond)
Call an IBCLC if:
- pumping hurts or causes nipple damage
- you’re unsure about flange size
- output is persistently low despite schedule and good setup
- you’re triple feeding and burning out
- you want an exclusive pumping plan tailored to your baby and goals
Contact your healthcare provider promptly if:
- fever/chills/flu-like symptoms with breast pain (possible mastitis)
- worsening redness, swelling, or severe pain
- signs of infection on nipples
- you feel emotionally overwhelmed in a way that feels scary or unsafe
FAQs
If exclusively pumping, many aim for 8–12 sessions per 24 hours early on. If pumping alongside nursing, 1–2 pumps/day or pumping when a feed is missed is common.
Common reasons include incorrect flange size, worn pump parts, inconsistent schedule, difficulty triggering letdown, stress/sleep deprivation, or a pump that isn’t strong enough for early postpartum needs.
Your nipple should move freely in the tunnel without rubbing, with minimal areola pulled in. Pain, swelling, blanching, or friction often suggests the wrong size.
Often 15–20 minutes, or until flow slows plus a few minutes. If pain occurs, address flange size and suction first.
Yes. It’s real feeding work. Systems—like a pumping station and drying workflow—make it more sustainable.
Absolutely. Combo feeding can protect your mental health and sleep while still providing breastmilk benefits. See Newborn Combo Feeding.
Related Reads
For all newborn feeding paths and checklists, start at the Feeding Hub.
If you’re new to newborn feeding patterns and cues, read How to Survive Newborn Feeding?
If you’re mixing breastmilk and formula (or doing breast and bottle), our combo feeding guide is here: Newborn Combo Feeding







